Endovascular Therapy of Acute type B Aortic Dissection Complicated with Visceral Malperfusion
Huang Cheng, Liu Yuan, Luo Songyuan, Feng Yingqing, Huang Wenhui and Luo Jian fang
DOI10.21767/2573-4482.18.03.6
Department of Cardiology, Guangdong General Hospital, Guangdong Cardiovascular Institute, Dongchuan Road 96#, Guangzhou, 510080, China
- *Corresponding Author:
- Luo Jian fang
Department of Cardiology, Guangdong General Hospital
Guangdong Cardiovascular Institute, Dongchuan Road 96#, Guangzhou, 510080, China.
Tel: 020-83827812
E-mail: luo_henry@qq.com
Received date: March 08, 2018; Accepted date: April 06, 2018; Published date: April 19, 2018
Citation: Cheng H, Yuan L, Songyuan L, Yingqing F, Wenhui H, et al. (2018) Endovascular Therapy of Acute type B Aortic Dissection Complicated with Visceral Malperfusion. J Vasc Endovasc Therapy. 3:6. doi: 10.21767/2573-4482.100076
Abstract
Organ ischemia owing to aortic dissection often requires emergency surgery for rapid restoration of blood flow into true lumen. We here present a case of 54 years old woman who was admitted to our hospital and underwent TEVAR. The pre-procedural course was complicated by visceral ischemia, which led to renal dysfunction, metabolic acidosis, and paralyzed intestinal obstruction. The case reported suggests that TEVAR is a viable treatment in the management of Standford type B Debakey III aortic dissection complicated with organ malperfusion.
Keywords
Standford type B Debakey III aortic dissection; Thoracic endovascular aortic repair TEVAR; Malperfusion; Visceral ischemia
Introduction
Visceral organ ischemia is serious complication of acute aortic dissection, and delayed diagnosis can be lethal. Patients with ischemia may present with abdominal pain or distention, or renal dysfunction.
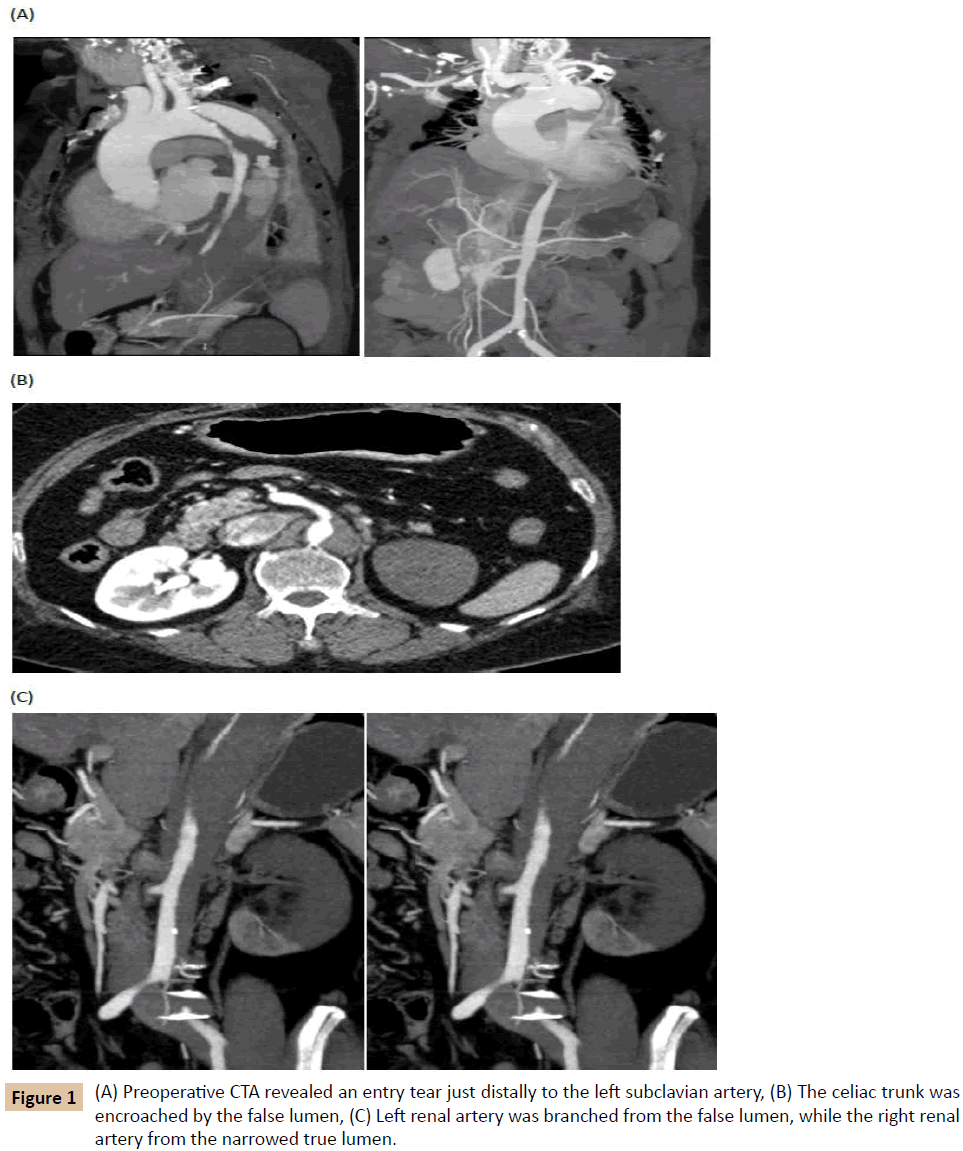
Malperfusion complication of aortic dissection is caused by true lumen obliteration of aortic artery and accompanied branches by high-pressured encroaching false lumen, thus reliable method to reestablish blood flow into the true lumen is necessary for improving organ perfusion. We here report a case of Standford type B, and Debakey type III aortic dissection, which was complicated by organ malperfusion and has been redressed by thoracic endovascular aortic repair (TEVAR), during which false lumen was identified only by aortic angiography, and a “chimney” stent has been installed into the left subclavian artery (LSA) to facilitate proximal landing of the aortic stent graft (Figure 1A-C).
Case Report
A 54 year old woman with past medical history of untreated hypertension, untreated diabetes mellitus was admitted to our hospital with severe chest and back pain for one day. Upon arrival, the patient underwent computed tomographic angiography (CTA), which showed acute aortic dissection of Standford type B, and Debakey type III, initiating just distally to the left subclavian artery and prolonging to the left common iliac artery. The highly-pressurized bulging false lumen encroached on the central lumen of the aorta, as well as the celiac trunk and the left renal artery. Apart from leukocytosis, the laboratory findings were remarkable.
Initial laboratory data was significant for white blood cell count of 27.37*109/L, creatine of 346.0 umol/L, CO2 combining power down to 17.7 mmol/L, and a normal potassium level. The pulsations of left femoral and dorsalis pedis artery were weak, without obvious ischemic discoloration of the corresponding limb.
The third day after admission morning laboratory data showed further decline in her creatinine to 586.28 umol/L, elevated lactic acid of 2.3 mmol/L, and a worsening CO2 combining power down to 15.9 mmol/L, indicative of metabolic acidosis. Further, the patient demonstrated clinical manifestations such as abdominal distention, nausea, vomiting, weak bowel sound, which is consistent with progressive visceral ischemia, as evidenced by diffuse ilius and gaseous distention on plain abdomen radiography. Hemodialysis, gastrointestinal decompression, extra gastrointestinal nutrition and antimicrobial treatment have been conducted. After extensive discussion of risks versus benefits of endovascular repair (EVAR) and conservative treatment, she opted for TEVAR. To block the proximal entry tear and to restore true lumen blood flow, a Xianjian ankura 34/28*200 mm tapered covered stent graft has been advanced just distally to the LSA. To facilitate proximal landing, LSA has been covered. Therefore, a fluency plus vascular 12*40 mm stent graft was advanced into LSA, the tip of which is paralled with that of the aortic stent graft.
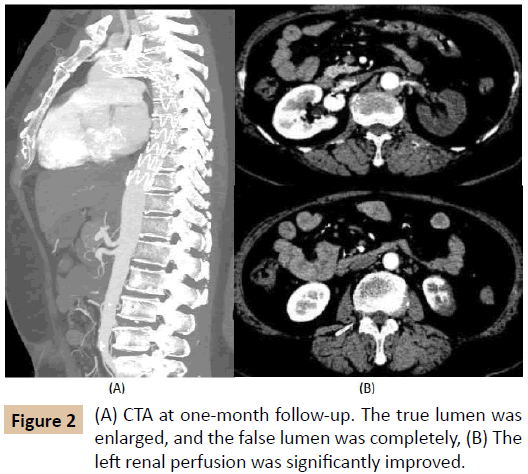
The patient demonstrated a good clinical course after TEVAR, with serum creatine decreased to 99.22 umol/L without the need for postoperative hemodialysis, white blood cell count dropped down to 6.12*109/L, and CO2 combining power rise to 21.6 mmol/L on postoperative day 7, and without any complaint of fever, nausea, vomiting, diarrhea, dizziness, chest or abdominal pain, paralysis. A one-month follow-up enhanced CT examination showed the TEVER was successful indicated by demonstrating an increment of true lumen size, thrombosis of the false lumen, and absence of bowel ischemia. No endo-leakage of any subtype has been detected (Figure 2A and B).
Discussion
Aortic dissection can place patients at risk for organ ischemia, which can start at the onset of dissection or later in the disease course and have lethal sequelae. Endovascular stent grafting as an alternative to conventional surgical repair for aortic dissection was first advocated in 1999, and is has currently been the preferred means of coping with distal malperfusion in acute complicated aortic dissection of Standford type B [1,2]. Through a surgical incision, a synthetic covered stent is delivered via the common femoral artery into the aorta and advanced to seal the proximal entry tear, thus may improve distal perfusion immediately through obliterating encroachment of the true lumen by the false lumen and initiating thrombosis of the false lumen.
Although EVAR has emerged as the standard strategy of coping with Type B aortic dissection complicated with distal malperfusion, complications related to stent grafting, including cerebral and spinal cord ischemia, continue to challenge endovascular procedures. Of note, coverage of the LSA during TEVAR has been independently associated with increased rates of stroke and peri-operative mortality [3]. Therefore, maintained perfusion of the LSA is imperative. In this case, a "chimney" stent has been placed into the LSA, and on one-month followup, the patient complained no dizziness, no paralysis. Further, intravascular ultrasound (IVUS) is often used for distinguishing true and false lumens [4], whereas in our case, only aortic angiography has been performed to identify the false lumen [4].
Despite the limitations of being a case study, our case documents a patient with malperfusion involvement of intestines and left kidney as a consequence of dissection demonstrated reversal of apparent paralytic ileus and renal dysfunction after TEVAR. Although the long-term benefits of TEVAR for acute complicated type B aortic dissection remain to be elucidated, the rapid nature and relatively low morbidity rate appear to highlight it as a promising treatment for complicated acute type B dissections.
References
- Nicholas A, Jeffrey K, Asvin G (2014) Current management and outcome of chronic type B aortic dissection: results with open and endovascular repair since the advent of thoracic endografting. Ann Cardiothorac Surg 3: 264-274.
- Chang L (2017) Endovascular Repair in Acute Complicated Type B Aortic Dissection: 3-Year Results from the Valiant US investigational Device Exemption Study. Korean J Thorac Cardiovasc Surg 50: 137-143.
- Ryan C, Virgas L, Mastracci (2013) Progress in management of malperfusion syndrome from type B dissections. J Vasc Surg 57: 1283-1290.
- Bao G, Zhen S, Da G (2015) Effect of Intravascular Ultrasound-assisted Thoracic Endovascular Aortic Repair for “Complicated” Type B Aortic Dissection. Clin Med J 128: 2322-2329.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences