Infrageniculate Popliteal Artery Injury Due to Single Gunshot Penetrating Trauma
Stamatatos I, Dimitriadis I, Metaxas E, Lioumpas D, Ralli S, Ispanopoulou S, Tzagkarakis F, Georgoudi S, Minardos I, Anagnostopoulos G and Rogdakis A
DOI10.21767/2573-4482.19.04.5
1Department of Vascular and Endovascular Surgery, General Hospital Nikaia, Greece
2Department of General Surgery, General Hospital Nikaia, Greece
3Cardiothoracic Surgery Department, General Hospital Nikaia, Greece
4Anaesthesiology Department, General Hospital Nikaia, Greece
5Radiology and Imaging Department, General Hospital Nikaia, Greece
- *Corresponding Author:
- Ioannis Stamatatos
Department of Vascular and Endovascular Surgery
General Hospital Nikaia, Greece
Email: jeanhipp56@gmail.com
Received date: January 29, 2019; Accepted date: February 13, 2019; Published date: February 20, 2019
Citation: Stamatatos I, Dimitriadis I, Metaxas E, Lioumpas D, Ralli S, et al. Infrageniculate Popliteal Artery Injury Due to Single Gunshot Penetrating Trauma. J Vasc Endovasc Therapy. 2019, 4:1.
Copyright: © 2019 Stamatatos I, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Acute lower limb ischemia caused by penetrating vascular injury in the infrapopliteal fossa is uncommon in everyday practice and is associated with high amputation rates.
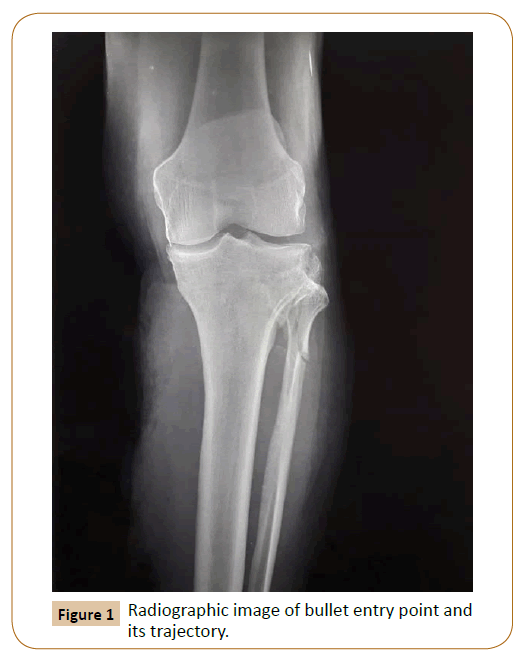
We report the case of a 62-year-old male with an infrageniculate popliteal penetrating arterial injury due to single gunshot trauma. The bullet entry wound was in the upper external tibial region, fractured the head and neck of the fibula bone, and transverse oblique posterior to tibial tuberosity, completely transecting the 3rd part of popliteal artery just above arterial trifurcation, and exiting in the middle medial calf region.
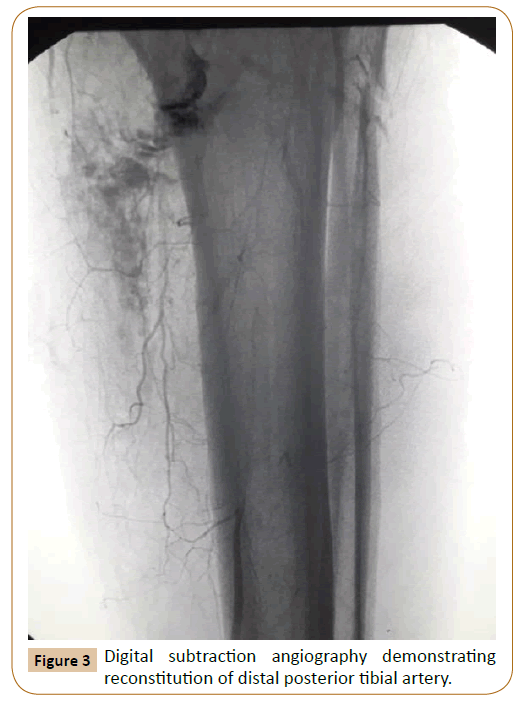
Digital subtraction angiography revealed completely arterial infrageniculate discontinuation with delayed collateral recanalization of posterior tibial artery in middle tibial region. The patient underwent emergency revascularization with the use of a reversed saphenous vein bypass graft. The patient had uneventful recovery and 6 months postoperatively at the follow up remains well with no reported complications.
Keywords
Penetrating arterial injury; Infrageniculate trauma; Peripheral vascular trauma
Introduction
Peripheral arterial injuries may result from penetrating or blunt trauma to the extremities. If not recognized and treated rapidly, may have disastrous consequences resulting in the loss of life and limb. The incidence of arterial injuries below the popliteal fossa is difficult to determine because most of these injuries, when isolated, cause no vascular compromise. Acute lower limb ischemia caused by penetrating vascular injury in the infrapopliteal fossa is uncommon in everyday practice and is associated with high amputation rates.
Case Presentation
A 62-year-old male patient presented in the emergency department due to penetrating left lower limb gunshot injury. He was tachycardic but normotensive with no signs of active external bleeding. Bullet entry wound was in the upper external tibial region, fractured the head and neck of the fibula bone, and transverse oblique posterior to tibial tuberosity, completely transecting the 3rd part of popliteal artery just above tibioperoneal trunk, and exiting wound located in the middle medial calf region (Figure 1).
Clinically reduced mobility and par aesthesia with coolness was noticed. Popliteal and tibial arteries below the knee were nonpalpable, whereas arteries of the contralateral lower limb were palpable throughout its entire length. Hand Doppler device revealed a monophasic waveform through the posterior tibial artery at the level of medial malleolus, with an ankle brachial index (ABI) of 0.20.
Patient underwent an emergency digital subtraction angiography (DSA) which demonstrated occlusion of the 3rd part of popliteal artery with evidence of thrombosis associated with injury and distal posterior tibial artery reconstitution from poor collateral flow (Figures 2 and 3).
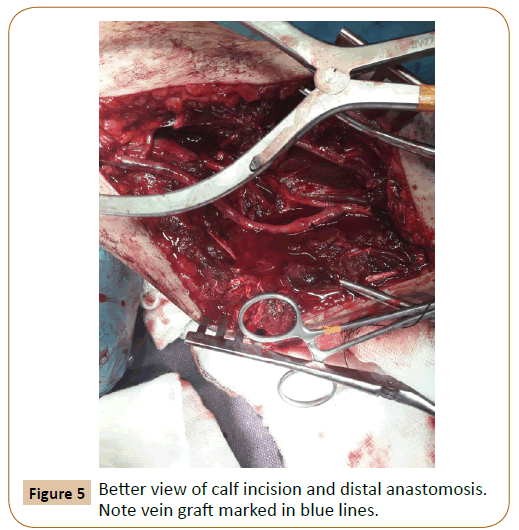
Emergency operation and revascularization of the ischemic limb was performed with constitution of a femoral to posterior tibial bypass graft with the use of great saphenous vein from the contralateral limb (Figures 4 and 5). After completion of the bypass an anterior compartment fasciotomy of the calf was performed. Immediately postoperatively the limb regained its warmness and a strong biphasic Doppler pulse signal appeared in posterior tibial artery which by postoperative day 2 was palpable.
The patient received IV heparin (target 60<aPTT<90) for 14 days and then started coumarin anticoagulant per os (target 2<INR<3) which continues for life. Neurological examination of the limb was intact, fasciotomy closure performed on day 19 and he was discharge on day 21 prescribing physical therapy sessions.
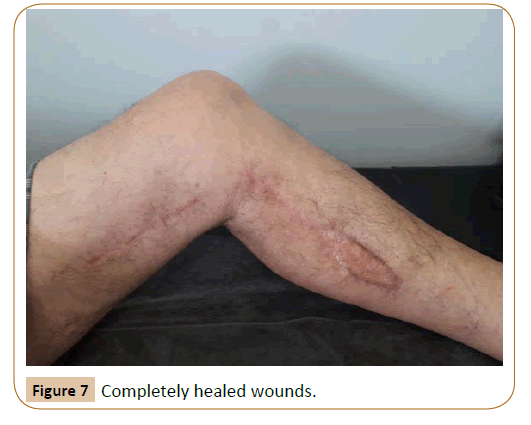
The patient short after returned to his previous activities was completely uneventful at 6 months follow up (Figures 6 and 7) and he is monitored outpatient regularly.
Discussion
Peripheral vascular injuries account for 80% of all cases of vascular trauma, and the great majority of patients are young males.
Most of the injuries involve the lower extremities and are caused by high-velocity weapons (70% to 80%), followed by stab wounds (10% to 15%) and blunt trauma (5% to 10%) [1-3].
The overall incidence of vascular injuries to the extremities is increasing accounting in modern series in 0.5% to 1% of injured patients but occurring in 20% to 50% of all vascular injuries [4,5].
One large study analyzing 755 patients sustaining gunshot wounds below the knee reported 136 injuries below the popliteal fossa identified on angiography-an incidence of 18% [6].
The most common arterial lesions are partial/ incomplete transection, transection and contusion of the vascular wall. Usually complete transection leads to arterial spasm and thrombosis with subsequent ischemia of the end organ, while partial transection usually causes persistent bleeding or false aneurysm formation [7].
Patients with blunt injuries experience mortality rates between 2% and 5%, whereas penetrating injuries generally result in fewer deaths [8].
Amputation rates in patients with extremity vascular injury range from 7% to 30%, with the most amputations performed in patients with blunt mechanisms [9].
Popliteal artery is the most frequently injured artery in the lower extremity by blunt trauma and the superficial femoral artery most frequently injured in penetrating trauma [8].
In penetrating trauma, bone fractures are seen in only 15% to 40% of limbs with an arterial injury while in blunt limb trauma, fractures are rated as high as 80% to 100% [10].
A European six years study findings of an urban trauma centre strongly correlated the presence of either major nerve or bony injury with limb loss [11].
The presence of a significant soft tissue deficit does appear to correlate with high rate amputation in lower extremity arterial trauma [8,10,12].
Although patients with multiple tibial artery injury should not be denied revascularization, expectations for limb salvage in both the short-term and long-term periods should be carefully outlined [13].
Conflict of Interest
None
References
- Rich NM, Spencer FC (1978) Vascular Trauma. WB Saunders Philadelphia, PA.
- Oller DW, Rutledge R, Clancy T, Cunningham P, Thomason M, et al. (1992) Vascular injuries in a rural state: a review of 978 patients from a state trauma registry. J Trauma 32: 740-746.
- Gupta R, Rao S, Sieunarine K (2001) An epidemiological view of vascular trauma in western Australia: a 5-year study. Aust N Z J Surg 71: 461-466.
- Loh SA, Rockman CB, Chung C, Maldonado TS, Adelman MA, et al. (2011) Existing trauma and critical care scoring systems underestimate mortality among vascular trauma patients. J Vasc Surg 53: 359-366.
- Perkins ZB, De'Ath HD, Aylwin C, Brohi K, Walsh M, et al. (2012) Epidemiology and outcome of vascular trauma at a British Major Trauma Centre. Eur J Vasc Endovasc Surg 44: 203-209.
- Ordog GJ, Balasubramanium S, Wasserberger J, Kram H, Bishop M, et al. (1994) Extremity gunshot wounds: I. Identification and treatment of patients at high risk of vascular injury. J Trauma 36: 358-368.
- Stamatatos I, Bouboulis K, Metaxas E, Klapsakis D, Anagnostopoulos G, et al. (2018) Damage Control and Staged Management in Zone 1 Vascular Abdominal Trauma. J Trauma Care 4: 1030.
- Tan TW, Joglar FL, Hamburg NM, Eberhardt RT, Shaw PM, et al. (2011) Limb outcome and mortality in upper and lower extremity arterial injury: a comparison using the National Trauma Data Bank. Vasc Endovasc Surg 45: 592-597.
- Kauvar DS, Sarfati MR, Kraiss LW (2011) National trauma databank analysis of mortality and limb loss in isolated lower extremity vascular trauma. J Vasc Surg 53: 1598-1603.
- Mullenix PS, Steele SR, Andersen CA, Starnes BW, Salim A, et al. (2006) Limb salvage and outcomes among patients with traumatic popliteal vascular injury: an analysis of the National Trauma Data Bank. J Vasc Surg 44: 94-100.
- Galyfos G, Giannakakis S, Geropapas G, Kastrisios G, Stefanidis G, et al. (2015) Arterial trauma of the limbs and pelvis: A 6-year experience of an urban trauma centre. Hellenic J Surg 87: 234-238.
- Wagner WH, Calkins ER, Weaver FA, Goodwin JA, Myles RA, et al. (1988) Blunt popliteal artery trauma: one hundred consecutive injuries. J Vasc Surg 7: 736-743.
- Liang NL, Alarcon LH, Jeyabalan G, Avgerinos ED, Makaroun MS, et al. (2016) Contemporary outcomes of civilian lower extremity arterial trauma. J Vasc Surg 64: 731-736.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences