Innominate Artery Pseudo-aneurysm: A Novel Hybrid Approach
Tal Assa, Alexander Belenky, Eli Atar, Guy Refaeli, Sergey Litvin and Basheer Sheick Yousif
DOI10.21767/2573-4482.18.03.7
Rabin Medical Center, Israel
- *Corresponding Author:
- Basheer sheick yousif
Senior Vascular Surgeon, Rabin Medical Center, Israel.
Tel: 0528172999/099620700
E-mail: basheersh@clalit.org.il
Received date: March 29, 2018; Accepted date: April 19, 2018; Published date: April 30, 2018
Citation: Assa T, Belenky A, Atar E, Refaeli G, Litvin S, et al. (2018) Innominate Artery Pseudo-aneurysm: A Novel Hybrid Approach. J Vasc Endovasc Therapy. 3:7 doi: 10.21767/2573-4482.100077
Abstract
We will describe a case of an innominate artery pseudo-aneurysm treated in a hybrid fashion. This is an interesting case of an 80-year-old man who underwent a PET-CT as part of bacteremia work-up. Initially suspected ascending aorta aneurysm was later confirmed to be a pseudo-aneurysm arising immediately distal to the innominate artery base by CTA imaging. Facing the aneurysm’s risky and rapidly evolving nature, the challenging anatomy and the patient health condition - a creative solution was the only option.
Keywords
Innominate artery; Pseudoaneurysm; Minimally invasive; Hybrid; Proximal neck
Introduction
Innominate artery (IA) aneurysms account for approximately 3% of all arterial aneurysms. Analogous to other aneurysms, they might cause local compression, thrombosis or distal embolization, giving rise to a diverse range of symptoms including dyspnoea, dysphagia, hoarseness, facial and upper right limb oedema, chest pain, digital ischemia, right hemispheric symptoms, amorosis fugax, vertebrobasilar syndrome, and rarely the presence of a pulsatile anterior thoracic mass [1].
In the past, treatment of these challenging surgical problems had consisted of aneurysm resection and interposition grafting, an invasive and complicated procedure [2].
A more recent approach for a lot of these complicated aneurysms treatment is with hybrid surgical and endovascular treatment. The hybrid procedures, however, still include complicated surgical manipulations with their obvious complications [3].
Endovascular stent-graft implantation is an alternative to open surgical repair in high-risk patients or special circumstances with only few cases described in the literature [4].
Case Report
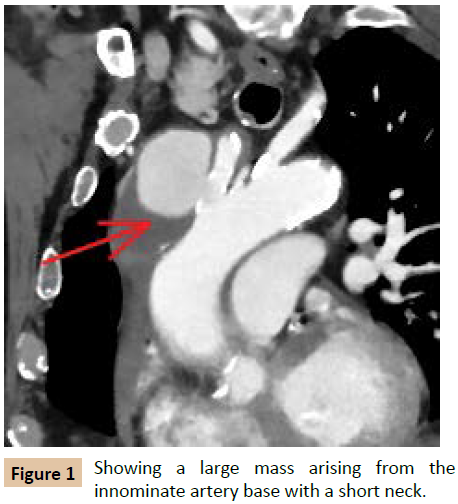
An 80-year-old man with multiple previous illnesses was recently hospitalized in another facility for MRSA bacteremia treatment. There, he was treated with I.V. antibiotics and the removal of his cardiac pacemaker. A CTA scan, due to a suspected pulmonary embolism (which was excluded) revealed a novel infiltration surrounding the ascending aorta - without any sign of active leakage. Two months later, in our hospital, as part of the bacteremia work-up he underwent a PET-CT which did not demonstrate a specific inflamed region but was immediately followed by a CTA scan (Figure 1) due to a large (55 X 73 X 47 mm) mass detected in the ascending aorta, near the origin of the innominate artery, suspected to be a pseudo-aneurysm with a large mural thrombus inside.
Although the aneurysm was asymptomatic (i.e. no chest pain or dysphagia etc.) treatment was imperative. The size, complicated location adjacent to the aorta arch, rapid evolvement and possible infection involvement - all contribute to a higher risk of rupture or distal embolism. Moreover, the short neck excluded the possibility of hermetic stent graft fixation and sealing. Considering all the above, and regarding the patient’s poor health condition, a multidisciplinary team including vascular surgeons and invasive radiologists, decided that the best solution would be an endovascular one. Due to its relative rarity and difficult anatomy (i.e. short neck and a large aneurismal base) a creative solution was proposed.
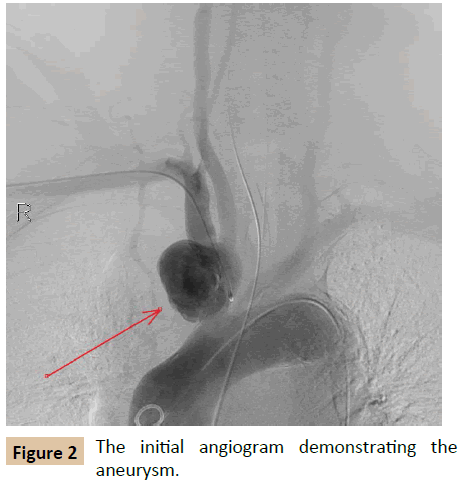
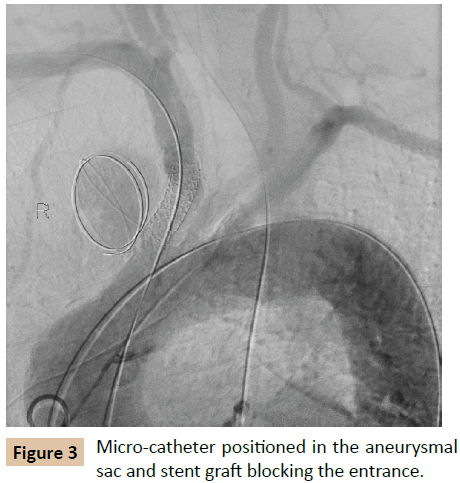
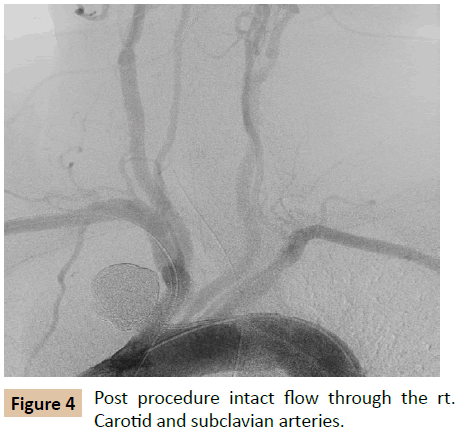
In the operation suite, under a general anesthesia and full heparinization (ACT=250s), both femoral arteries were percutaneously accessed and the left brachial artery was exposed surgically. Then, an angiogram was obtained, demonstrating the above mentioned aneurysm (Figure 2). A PROGRAET 2.4F micro-catheter (TERUMO, Tokyo, Japan) was inserted into the aneurysmal sac using a SYNCHRO 14 micro-guide (STRYKER Neurovascular, Cal, US). Then, two 8 X 38 mm + 10 X 38 mm ADVANTA V12 (ATRIUM, Hud, US) stent grafts were placed blocking the pseudo-aneurysm neck (Figure 3). 10 AXIUM 3D coils (EV3 Endovascular, Ply, US) ranging between 25 mm to 12 mm and 10 TRUFILL 10 X 100 mm (CODMAN, MA, US) were implanted in the aneurysmal sac. Due to the graft's location, an attempt to use SPIDER FX protection device (EV3 Endovascular, Ply, US) was unsuccessful, therefore an occlusion test was performed using an inflated 12 X 40 mm balloon in the stent graft and an angiogram of the cerebral vasculature through the left femoral access - demonstrating a good distribution. Then, ONYX 34 (EV3 Endovascular, Ply, US) in a total volume of 15 ml was injected under the constant intermittent inflation of the stent graft with a balloon to avoid any leakage, displacement and embolism of the ONYX and the coils. Finally, angiograms were taken, demonstrating a complete sealing of the aneurysm and intact flow through the right carotid artery (Figure 4).
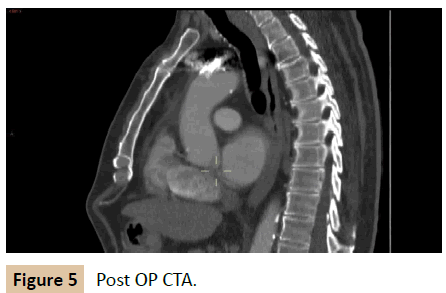
Post operation CTA was performed 2 months after the procedure and showed a patent innominate artery with a sealed aneurysm (Figure 5).
Discussion
Since innominate pseudo-aneurysm is a rare, yet life threatening condition, and reports on surgical and endovascular treatment options are limited, a multidiscipline innovative approach should be taken in each new case.
In the past, treatment of such aneurysms involved a major operation with a median sternotomy or thoracotomy causing a myriad of complications such as stroke and death. Different groups reported hybrid endovascular treatments of aneurysms in the innominate artery, among them several true aneurysms [5] and ruptured mycotic aneurysm [4]. All of the above either used a surgery or multiple operations.
The common denominator of the different recent approaches is the avoidance of major thoracic operation.
Only few case reports described a pure endovascular treatment for such aneurysms with promising results, yet, to the best of our knowledge, no large series with long follow-ups where conducted [3].
To deal with such a complex aneurysm as in our case, with all the above mentioned potential risks, our team of experts - which included a thoracic surgeon and interventional radiologists - co - operated in tailoring the optimal and safest procedure.
Our main goal was to exclude the dangerous aneurysm while avidly protecting the brain from embolic events during and post procedure.
Here we have described a minimally invasive endovascular procedure which included 2 steps in one operation approach, and was proven to exclude the large innominate aneurysm which had no proximal neck, with a protection from leakage and embolization of coils and sealant materials - all the above without compromising neither the right carotid nor the right subclavian arteries.
We hope that this multidisciplinary innovative technique and minimal invasive approach in general, will guide further similar cases treatment and be improved with the accumulation of knowledge and experience.
References
- Erdinc Soylu (2013) Surgical treatment of innominate artery and aortic aneurysm: a case report and review of the literature. J Cardiothorac Surg 8: 141.
- Cherry K (2006) Treatment of extracranial, carotid, innominate, subclavian and axillary aneurysms.
- Domenico Angiletta (2012) Eight-year follow-up of endovascular repair of a brachiocephalic trunk aneurysm due to Takayasu's arteritis. JVS 56: 504-507.
- Bush R, Hurt J, Bianco C (2002) Endovascular management of a ruptured mycotic aneurysm of the innominate artery. Ann Thorac Surg 74: 2184-2186.
- Van Leemputa A, Maleuxa G, Heyea S, Nevelsteenb A (2007) Combined open and endovascular repair of a true right subclavian artery aneurysm without proximal neck. Interact CardioVasc Thorac Surg 6:406-408.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences