Catheter Directed Thrombolytic Therapy for Acute Deep Vein Thrombosis-Our Experience
Harivadan Lukka, Aditya Nutakki and Manitha Kondru
DOI10.21767/2573-4482.20.05.15
1Assistant Professor, Department of Cardiothoracic and Vascular Surgery, Andhra Medical College, Visakhapatnam, India
2Associate Professor, Department of Radio-diagnosis, Gayatri Vidya Parishad Institute of Health Care and Medical Technology, Visakhapatnam, India
- *Corresponding Author:
- Harivadan Lukka
Assistant Professor
Department of Cardiothoracic and Vascular Surgery
Andhra Medical College, Visakhapatnam, India
Tel: +9849849454
E-mail: dr_harivadan@yahoo.com
Received Date: June 16, 2020; Accepted Date: June 24, 2020; Published Date: July 01, 2020
Citation: Harivadan L, Aditya N, Manitha K (2020) Catheter Directed Thrombolytic Therapy for Acute Deep Vein Thrombosis-Our Experience J Vasc Endovasc Ther. Vol. 5 No. 3: 15.
Abstract
Objectives: The objective of this study is to ascertain that the catheter directed thrombolytic therapy for acute deep vein thrombosis results in significant reduction in the thrombus burden while minimizing the systemic thrombolytic effects.
Materials and Methods: This was a retrospective cross-sectional study carried out in the department of Cardiothoracic and vascular Surgery from September 2016 to February 2020. All the patients included in this study were taken from the Medical records of the hospital considering International Classification of Diseases code.
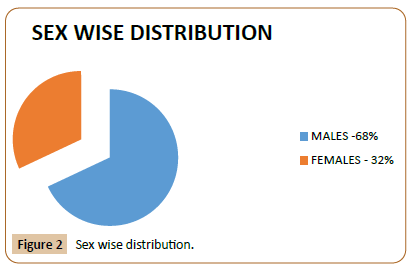
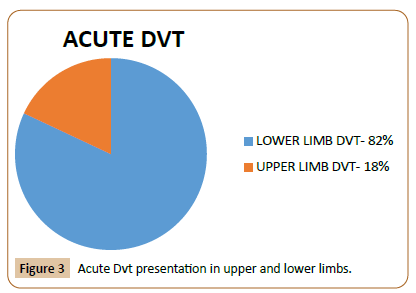
Results: This was a 4-year retrospective study and total number of 100 patients were included in the study. Males contributed to 68% and 32% females. 82 % of the total cases of acute deep vein thrombosis of lower limbs and 18 % are of upper limb deep vein thrombosis. Acute deep vein thrombosis (DVT) within 14 days of presentation are included in this study. The age group between 20 years and 86 years are included with average age being 43.2 years. Provoking factors were found in 12 cases as May thurner’s Syndrome.
Conclusions: Acute deep vein thrombosis is a common disease and is associated with complication of Post thrombotic syndrome (PTS) and Pulmonary thromboembolism( PTE). Catheter directed thrombolytic therapy of acute deep vein thrombosis is associated with decreased thrombus burden and maintenance of the vein valve patency which prevents progression into Post thrombotic Syndrome.
Keywords
Deep vein thrombosis; Catheter directed thrombolytic therapy (CDTT); Post thrombotic syndrome; Pulmonary thromboembolism; International classification of diseases code-ICD code
Introduction
Conventional treatment of Acute Deep vein thrombosis is with Antithrombotic therapy starting with intravenous unfractionated heparin or subcutaneous low molecular weight heparin followed by oral anticoagulation with vitamin K antagonists [1]. The conventional anticoagulation prevents the expansion and progression of thrombus, pulmonary thrombo-embolism and death from venous thrombo-embolism. Approximately half of the patients with proximal Deep vein thrombosis develop symptoms of Post Thrombotic Syndrome (PTS) and one fourth with proximal Deep vein thrombosis develop chronic post thrombotic complications are severe. Trials have demonstrated that proper use of graduated Compression stockings reduces the risk of PTS morbidity by 50% [2,3]. PTS complications of acute deep vein thrombosis are because of the persistent venous obstruction and destruction of the function of the vein valve [4,5]. Catheter directed thrombolytic therapy is loco-regional delivery of thrombolytic dose directly to the venous thrombus, resulting in significant reduction of the thrombus burden with minimal systemic thrombolytic effect.
Material and Methods
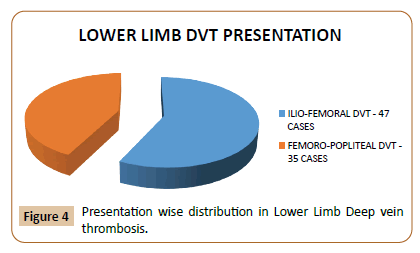
This was a retrospective cross-sectional study carried out in the department of Cardiothoracic and vascular Surgery from September 2016 to February 2020. All the patients included in this study were taken from the Medical records of the hospital considering International Classification of Diseases code. Deep vein thrombosis was identified by duplex ultra-sonography and computed tomography venogram Wherever required. PTE was identified by CT angiogram. The levels of Deep vein thrombosis was classified as Ilio-femoral, femoro-popliteal and tibial. The thrombo-check workup was not done for all patients. Tibial deep vein thrombosis was excluded in our study.
Results
This was a 4-year retrospective study and total numbers of 100 patients were included in the study. Males contributed to 68% and 32% females. 82 % of the total cases of acute deep vein thrombosis of lower limbs and 18 % are of upper limb deep vein thrombosis. Symptomatic patients with acute deep vein thrombosis (DVT) within 14 days of presentation are included in this study. Provoking factors were found in 12 cases as May thurner’s Syndrome.
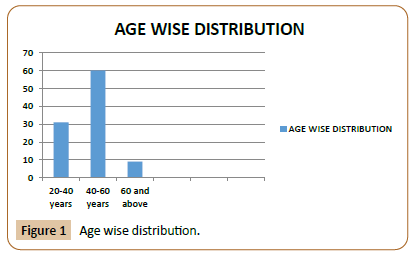
Age/Sex Wise Distribution
The age group between 20 years and 86 years are included with average age being 43.2 years. The peak incidence of Acute deep vein thrombosis was observed as 61 cases in our study between the age groups of 40-60 years (Figures 1-4).
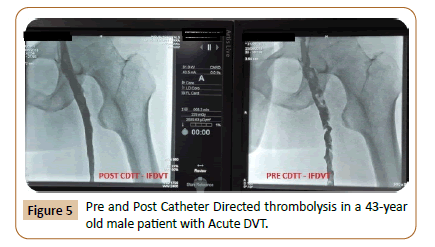
Cather directed thrombolytic therapy was done in all 100 cases. In this study the mean duration of symptoms was 8.47 days before procedure was undertaken. Lower limb CDTT is done in 82 % cases whereas 18 % CDTT is done in the Upper limb DVT. Mean dose of Thrombolytic used was 36 mg and the mean duration of infusion was 38 hours. 68 patients of acute DVT of lower limb achieved lysis of more than 50% with Villalta Score of them was an average of 4, whereas in 14 patients of acute DVT of lower limb achieved lysis of less than 50% and of them the average villalta score was 9. Non-major bleeding was present in 4 patients in our study (Figure 5).
Discussion
In this study we have retrosceptively analysed data of about 100 patient of acute deep vein thrombosis. This study looked primarily at symptomatic DVT with lower and upper limb pain and swelling presenting with pulmonary thrombo-embolism as main presenting feature and not the isolated Pulmonary thromboembolism. Males in our study contributed to 68% while in Indian Subgroup of Endorse and the Arrive study they contributed to 69% and 70% of the patient load [4-6].
The age-group between 41-60 years contributed the maximum cases of DVT in our study 61 cases and the mean age is 43.2 years ad it correlated with the Arrive study with a contrast to a population study conducted by Mayo Clinic in which the mean age was 61.7 years which suggests that DVT occurs in much younger age groups in Indians compared to Western [7].
By reviewing the success of thrombolysis, it was noticed that complete lysis was achieved in 71% patients. These results were comparable to that mentioned by Gomaa Et al., who reported that complete lysis was achieved in 82.2% patients and partial lysis in 14.3% patients [8]. Our results were compraible to the studies By Chang Et al., Sillesen et al., Enden et al., Elsharawy and Elsayat who mentioned complete lysis that was achieved in 80%, 93%, 88.9%, 61% respectively [9-12]. The Recent CaVent trail had mean clot resolution of 82%, whereas our study showed 71% complete resolution.
The mean duration of symptoms was 8.47 days in our study, comparable to Casey Et al. who stated that there was no significant effect of duration between the onset of symptoms and the time of delivering intervention within 14 days of onset [13]. The Society of Vascular Surgery and American venous forum accepted 14 days as the Cut off for CDTT in DVT treatment [14].
During our current study, 4 patients presented with clinically relevant non major bleeding which is less than that found by Gomaa and Colleagues [8] and CaVent trail [15].
Watson et al found that thrombolysis offers potential advantages over conventional treatment by reduction in the thrombus burden and the incidence of PTS in long term particularly in Iliofemoral DVT.
The Recent CaVent Trial showed that patients at 6 months follow up showed improved Ilio-femoral patency and less post thrombotic syndrome.
The Largest Attract Trial demonstrates significantly higher bleeding in CDTT group and no significant difference in post thrombotic syndrome at 2 years when compared to anticoagulation group alone which is 47% and 48% respectively [16]. This difference could be attributed to the difference in the duration of follow up of the patients in the larger population study when compared to the smaller population studies.
Ongoing randomized control trial-Dutch Cava Trial comparing the catheter directed thrombolytic therapy group vs. anticoagulation alone for the proximal deep vein thrombosis may provide more clinical evidence for the benefit of catheter directed thrombolytic therapy [17].
Conclusion
Catheter directed thrombolytic therapy in the setting of acute deep vein thrombosis was safe and tolerated by most of our patients, in a way to decrease in complications of Post thrombotic syndrome, improving the quality of life of the patients. This study evaluates only one modality of treatment, additional comparative studies with other modalities of treatment to clarify the potential risks and benefits of this treatment approach.
Financial Support and Sponsorship
Nil.
Conflicts of Interest
There are no conflicts of interest.
References
- Büller HR, Agnelli G, Hull RD, Hyers TM, Prins MH, et al. (2004) Antithrombotic therapy for venous thromboembolic disease: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest 126: 401S-428S.
- Prandoni P, Lensing AW, Prins MH, Frulla M, Marchiori A, et al. (2004) Below-knee elastic compression stockings to prevent the post-thrombotic syndrome: a randomized, controlled trial. Ann Intern Med 141: 249-256.
- Brandjes DP, Buller HR, Heijboer H, Huisman MV, Rijk M, et al. (1997) Randomized trial of effect of compression stockings in patients with symptomatic proximal-vein thrombosis. Lancet 349: 759-762.
- Lee A D, Stephen E, Agarwal S, Premkumar P (2009) Venous thrombo-embolism in India. Eur J Vasc Endovasc Surg 37: 482‑485.
- Pinjala R, ENDORSE-India Investigators (2012) Venous thromboembolism risk & prophylaxis in the acute hospital care setting (ENDORSE), a multinational cross‑sectional study: Results from the Indian subset data. Indian J Med Res 136: 60-67.
- Kamerkar DR, John MJ, Desai SC, D silva LC, Joglekar SJ (2016) Arrive: A retrospective registry of Indian patients with venous thromboembolism. Indian J Crit Care Med 20: 150-158.
- Silverstein MD, Heit JA, Mohr DN, Petterson TM, O'Fallon WM, et al. (1998) Trends in the incidence of deep vein thrombosis and pulmonary embolism: A 25‑year population‑based study. Arch Intern Med 158: 585-593.
- Baldwin M, Moore H, Rudarakanchana N, Gohel M, Davies A (2013) Post thrombotic syndrome: a clinical review. J Thromb Haemost 11: 795-805.
- Comerota AJ (2010) Randomized trial evidence supporting a strategy of thrombus removal for acute DVT. Semin Vasc Surg 23: 192-198.
- Du GC, Zhang MC, Zhao JC (2015) Catheter-directed thrombolysis plus anticoagulation versus anticoagulation alone in the treatment of proximal deep vein thrombosis; a meta-analysis. Vasa 44: 195-202.
- Engelberger R, Spirk D, Willenberg T (2015) Ultrasound assisted versus conventional catheter-directed thrombolysis for acute iliofemoral deep vein thrombosis. Circ Cardiovasc Interv 8: 1-3.
- Lin P, Ochoa L, Duffy P (2010) Catheter-directed thrombectomy and thrombolysis for symptomatic lower-extremity deep vein thrombosis: review of current interventional treatment strategies. Perspect Vasc Surg Endovasc Ther 22: 152-163.
- Casey E, Murad M, Zumaeta-Garcia M, Elamin M, Shi Q, et al. (2012) Treatment of acute ilio-femoral deep vein thrombosis. J Vasc Surg 55: 1463-1473.
- Meissner M, Gloviczki P, Comerota A, Dalsing M, Eklof B, et al. (2012) Early thrombus removal strategies for acute deep venous thrombosis: clinical practice guidelines of the Society for Vascular Surgery and the American Venous Forum. J Vasc Surg 55: 1449-1462.
- Enden T, Haig Y, Kløw NE, Slagsvold CE, Sandvik L, et al. (2012) Long-term outcome after additional catheter-directed thrombolysis versus standard treatment for acute iliofemoral deep vein thrombosis (the CaVenT study): a randomised controlled trial. Lancet 379: 31-38.
- Ezelsoy M, Turunc G, Bayram M (2015) Early outcomes of pharmacomechanical thrombectomy in acute deep vein thrombosis patients. Heart Surg Forum 18: 222-225.
- https://clinicaltrials.gov/ct2/show/NCT00970619
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences