Migrated Pelvic Coil Causing Pulmonary Infarct in an Adult Female
Angel Guerrero and Rebecca G Theophanous
DOI10.21767/2573-4482.20.05.2
Department of Surgery, Division of Emergency Medicine, Duke University Medical Center, Durham, USA
- *Corresponding Author:
- Rebecca G Theophanous
Department of Surgery
Division of Emergency Medicine
Duke University Medical Center, Durham, USA
Tel: 3306515581 E-mail: rbectheo@gmail.com
Received Date: January 07, 2020; Accepted Date: February 21, 2020; Published Date: February 28, 2020
Citation: Guerrero A, Theophanous RG (2020) Migrated Pelvic Coil Causing Pulmonary Infarct in an Adult Female. J Vasc Endovasc Therapy, Vol.5 No.1:1
Abstract
Purpose: The migration of endovascular coils is a relatively rare complication, with few cases reported in patients with pelvic congestion syndrome. Additionally, the coil retrieval process has not been well described. Case report: A 39-year-old female with recent coil embolization of her left internal iliac and ovarian veins for pelvic congestion syndrome presented with one month of rightsided chest pain and dyspnea. Chest radiograph and computed tomography (CT) imaging revealed a migrated pelvic coil in the patient’s right main pulmonary artery with associated pulmonary infarcts and a small right pleural effusion. Interventional radiology successfully removed the coil piecemeal via a bilateral femoral access approach, resulting in significant symptom improvement and only a small piece of coil left in situ. Conclusions: Careful history should be obtained in patients presenting with chest pain or dyspnea, including recent procedures. Endovascular retrieval of the migrated coil was a successful and safe intervention in this patient, resulting in symptom resolution without the requirement of long-term anticoagulation or monitoring. The patient was also spared a more invasive open surgical procedure, which could lead to prolonged recovery times and increased complication risk.
Keywords
Migrated coil; Pelvic congestion syndrome; Pulmonary infarct
Introduction
Pelvic congestion syndrome is chronic pelvic pain caused by gonadal vein varicosities, worsened by prolonged standing, sexual intercourse, menstruation, or pregnancy. Multiparous women of reproductive age are at increased risk, and the overall prevalence is about 30% [1]. Venogram is the diagnostic gold standard, and potential treatments include hormone therapy, vasoconstrictive medications, or pelvic coil embolization [1,2]. It is possible but rare for a pelvic coil to migrate to the pulmonary vasculature, and the few cases reported typically do not describe removal of the coils, as patients were asymptomatic.
We present an adult female with pelvic congestion syndrome status-post coil embolization with chest pain and dyspnea, found to have a migrated pelvic coil in her right pulmonary artery.
Case Report
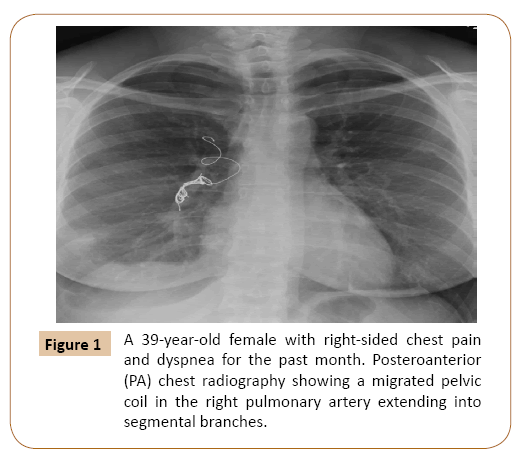
A 39-year-old female with pelvic congestion syndrome underwent coil embolization of the left internal iliac and ovarian veins three months prior. For the past month, the patient endorsed right-sided pleuritic chest pain and dyspnea with orthopnea. Outpatient chest radiograph demonstrated an ectopic coil in the right pulmonary vasculature, with a second coil still in place in the left ovarian vein.
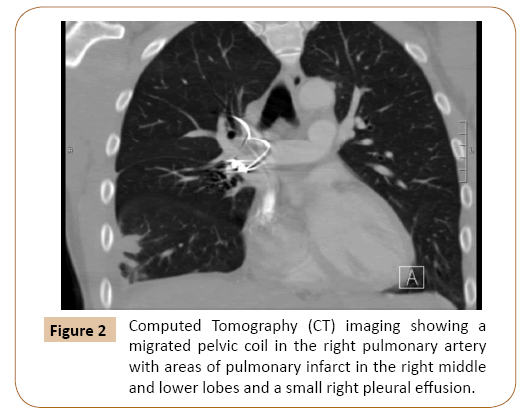
On Emergency Department evaluation, the patient had normal vitals including 100% oxygen saturation on room air, clear breath sounds, and no leg edema. Labs were unremarkable. Electrocardiogram demonstrated normal sinus rhythm. Chest radiograph and CT imaging revealed an ectopic pelvic coil in the right main pulmonary artery extending into multiple upper and lower lobe segmental branches (Figure 1). Coil artifact somewhat limited the identification of thrombus, but there were peripheral wedge-shaped opacities in the right middle and lower lobes concerning for infarcts and a small right pleural effusion (Figure 2). There was no evidence of right heart strain.
After much discussion between the patient’s medical providers, they decided that vascular interventional radiology (VIR) would be the least invasive yet still likely successful method for coil retrieval when compared to an open surgical approach. The patient was consented and transported directly to VIR, where the groin was prepped in standard fashion. The right common femoral vein was accessed with a micro puncture kit using ultrasound guidance. A pulmonary angiography catheter was advanced over a guide wire into the right main pulmonary artery via a 7 French sheath. Contrast phase did not show significant clot within the artery.
The sheath was exchanged for a long 7 French sheath with the tip in the right pulmonary artery. Multiple snares were passed through the sheath to engage the 20mm Nester coil pack (Cook Medical), however the coil unraveled into small pieces, until eventually a large piece was snared and retracted to the right femoral vein. VIR then performed en bloc removal through the right groin access site given the coil was too large to pass through the sheath; however, a piece of coil remained in the right femoral vein. Multiple attempts to snare the coil via an upsized 11 French sheath were still unsuccessful.
Similarly, the left femoral vein was accessed and upsized to a 9 French sheath, which finally allowed for successful snare removal of the remaining coil. Repeat imaging showed a small residual coil fragment in the right midlung that was deemed not to cause increased injury, thus was left in situ. An intact 16mm Nester coil pack was noted in the left gonadal vein.
The patient was observed in the hospital overnight and went home the following day without anticoagulation or other acute complications. The patient followed up with vascular surgery several months later for the remaining gonadal vein coil with no additional interventions.
Discussion
Coil embolization has been used since demonstrating efficacy in arterial occlusion in 1975 and in the treatment of pelvic congestion syndrome since first described by Edwards, et al in 1993 [2,3]. Current literature reports high symptomatic improvement rates of 70-85% for percutaneous vein embolization, whereas pharmacotherapy has had poor success in achieving pain relief [3]. Surgical ligation is another effective treatment but is much more invasive [1].
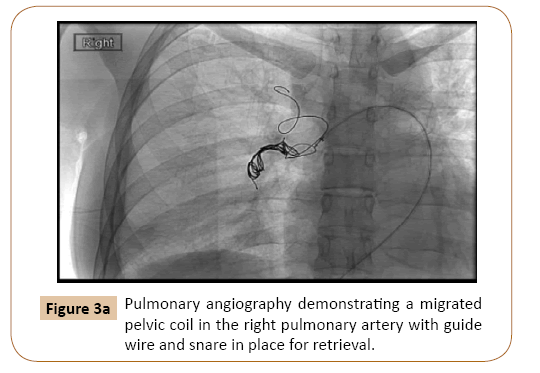
Complications of pelvic embolization include vein perforation and coil migration (either immediate or delayed) causing cardiac damage, arrhythmias, pulmonary infarct, and thrombophlebitis, with rates ranging from 4-8% [4-6]. Few cases have been reported regarding migration of pelvic coils to the pulmonary vasculature, and rarely with symptomatic patients requiring endovascular retrieval of the coils (Figure 3a) [7,8].
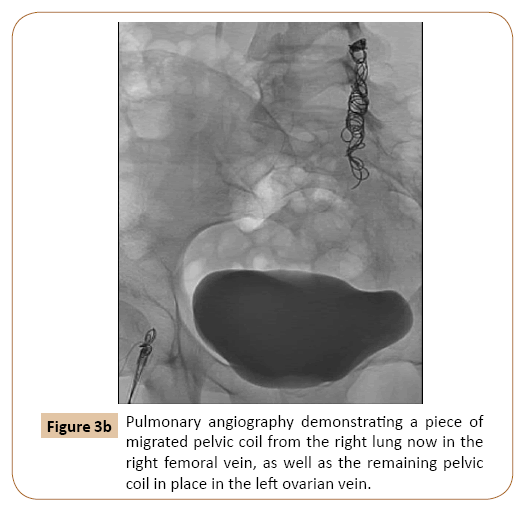
Yamasaki et al. described migration of nine internal iliac vein coils to the pulmonary artery, but the coils were not removed as the patient was asymptomatic. They, along with other studies, postulated that coils should be at least 30-50% the diameter of the target vessel in order to decrease migration risk. They also describe using coils with a stronger radial force, for example measuring 0.035 inch, as veins have lower frictional resistance (increased elasticity) between the vessel wall and the coils. Furthermore, larger vessels with a high-flow state (such as the internal iliac, as in our patient), are at higher risk for coil migration, especially when the varices are relieved and flow is increased [9]. Tonkin, et al. described two cases of coil migration to the tricuspid valve and pulmonary arteries with a coil fragment in the right ventricle, which were asymptomatic and conservatively managed [10] (Figure 3b).
None of these cases include removal of the coils nor the methods behind the retrieval process. Our patient developed pulmonary infarcts and a pleural effusion, which has not been previously reported, and thus necessitated urgent removal of the migrated coil, as we have described above. Although there were difficulties with VIR removal of the coil, this still prevented the patient from undergoing an open surgical procedure, which could lead to prolonged recovery time, longer hospital stay, and other post-operative complications such as non-healing wounds, infection, hemorrhage, pulmonary embolism, etc. Our patient had complete resolution of her symptoms and no additional complications on follow up.
Conclusion
The migration of endovascular coils is a relatively rare complication, with few cases reported in patients with pelvic congestion syndrome. Additionally, the coil retrieval process has not been well described. Careful history should be obtained in patients presenting with chest pain or shortness of breath, including recent procedures. Endovascular retrieval of the migrated coil was a successful and safe intervention in this patient, resulting in symptom resolution without the requirement of long-term anticoagulation or monitoring.
References
- Ignacio EA, Dua R, Sarin S, Harper AS, Yim D, et al. (2008) Pelvic congestion syndrome: diagnosis and treatment. Semin Interv Radiol 25: 361-368.
- Gianturco C, Anderson JH, Wallace S (1975) Mechanical devices for arterial occlusion. Am J Roentgenol 124: 428-435.
- Edwards RD, Robertson IR, MacLean AB, Hemingway AP (1993) Case report: pelvic pain syndrome-successful treatment of a case by ovarian vein embolization. Clin Radiol 47: 429-431.
- Maleux G, Stockx L, Wilms G, Marchal G (2000) Ovarian vein embolization for the treatment of pelvic congestion syndrome: long-term technical and clinical results. J Vasc Interv Radiol JVIR 11: 859-864.
- Ganeshan A, Upponi S, Hon LQ, Uthappa MC, Warakaulle DR, et al. (2007) Chronic pelvic pain due to pelvic congestion syndrome: the role of diagnostic and interventional radiology. Cardiovasc Intervent Radiol 30: 1105-1111.
- https://www.cathlabdigest.com/article/Coil-Embolization-Right-Side-Heart-After-Elective-Hypogastric-Vein-Embolization-Requiring.
- D'Amato R, Figueira JG, Palmero JT (2017) Pulmonary embolism due to metal coil migration after treatment of pelvic varices. Arch Bronconeumol Engl 53: 72.
- León FX, Alba B, Arribas A, García R, García I, et al. (2018) A rare case of pulmonary embolism due to endovascular coil embolization and review of literature. Int J Respir Pulm Med 5: 1-3.
- Yamasaki W, Kakizawa H, Ishikawa M, Date S, Tatsugami F, et al. (2012) Migration to the pulmonary artery of nine metallic coils placed in the internal iliac vein for treatment of giant rectal varices. Acta Radiol Short Rep 1: 1-4.
- https://www.atsjournals.org/doi/pdf/10.1164/ajrccm-conference.2018.197.1_MeetingAbstracts.A3700.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences