State of the Art on Endovascular Treatment of Renal Artery to Inferior Vena Cava Fistula following a Gunshot Injury
NN khanna, CT Nwagbara, A Nasar and DW Anggrahini
DOI10.21767/2573-4482.18.03.2
Department of Endovascular and Interventional Cardiology, Indraprastha Apollo Hospital, Delhi, India
- *Corresponding Author:
- CT Nwagbara
Department of Endovascular and Interventional Cardiology
Indraprastha Apollo Hospital, Delhi, India.
Tel: +919717669671
E-mail: chudidr@gmail.com
Received date: January 25, 2018; Accepted date: February 09, 2018; Published date: February 19, 2018
Citation: khanna NN, Nwagbara CT, Nasar A, Anggrahini DW (2018) State of the Art on Endovascular Treatment of Renal Artery to Inferior Vena Cava Fistula following a Gunshot Injury. J Vasc Endovasc Therapy. 3:2. doi: 10.21767/2573-4482.100072
Abstract
Traumatic fistula involving the renal artery and inferior vena cava is rare and it is usually as a result of penetrating injury. A case of right renal artery to inferior vena cava fistula following gunshot injury to the chest and upper thigh is reported. The hemodynamic change that usually follows these types of fistulae is also illustrated. We also describe the endovascular approach in the treatment of this condition.
Keywords
Endovascular treatment; Renal artery; Fistula; Gunshot injury
Introduction
Arteriovenous (AV) fistulae of the renal artery presents with a variety of hemodynamic changes. Penetrating injury to the abdomen is the most common cause of this condition. However, AV fistula involving the renal artery to inferior vena cava (IVC) is a rare condition. Early and prompt intervention in the treatment of this condition is the most important factor in preventing complications that arises from AV fistula involving the renal artery to inferior vena cava.
Case Report
A 36 year old male presented to our emergency department with 6 hours history of gunshot injury to the left side of chest wall and left upper thigh. The patient was initially taken to a nearby hospital where he was evaluated and found that he has high cardiac output heart failure, hemopericardium and hemothorax, he was resuscitated and Implantable Cardioverter Defibrillator (ICD) was placed before he was subsequently referred to our facility for further evaluation and management.
On admission, he was examined and found to be in severe respiratory distress, tachypneic and tachycardic. Some investigation where done which include Contrast-Enhanced Computed Tomography (CECT) of chest, CECT of the abdomen and 2 D echocardiography. Investigations revealed fistula communicating between the right renal artery and inferior vena Cava, high cardiac output of 8.5 litres per minute, hemothorax, and hemopericardium. The patient was initially managed conservatively at the intensive care unit and subsequently worked up for right renal artery to IVC fistula angioplasty and stenting.
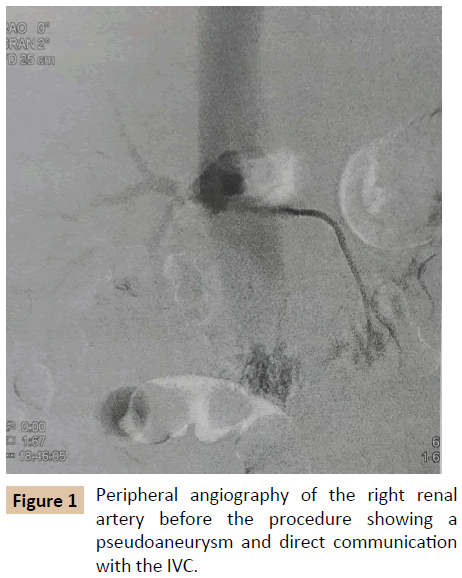
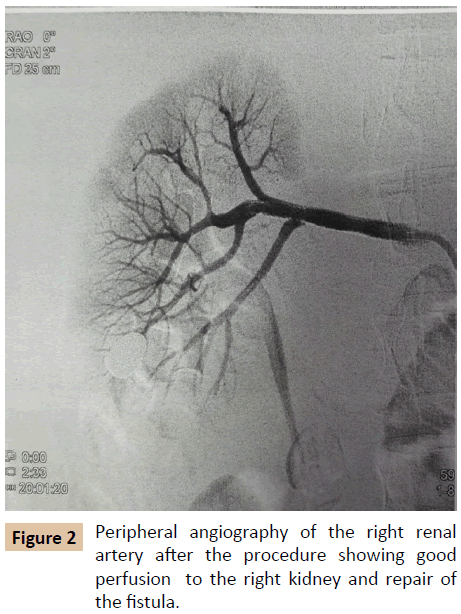
The patient was taken for percutaneous transluminal angioplasty and stenting to the right renal artery. A pre-procedure angiography showed a fistula of right renal artery to inferior vena cava and poor perfusion of the right kidney. The wire (0.035 x 260 cm Terumo wire, Europe) was passed into the right renal artery and 3 Abbott vascular graft master covered stents (4.50 mm x 26 mm, 4.50 mm x 19 mm and 4.00 mm x 19 mm, USA) were placed to the right renal artery. The graft was post dilated with Viatrac 14 plus 5.0 mm X 20 mm x 135 cm and Indigo 6.0 mm X 20 mm x 130 cm non complaiant balloons, India. The post procedure angiography was good and also there was good perfusion to the right kidney.
The patient improved after the procedure and their tachycardia and tachypnoiec returned to normal. A post-procedure echocardiogram showed a cardiac output of 4 liters per minute. Patient was discharged well on dual antiplatelet therapy.
Discussion
AV fistula between the right renal artery and IVC is usually follows a penetrating injury and is rare. An AV fistula is an abnormal communication between an artery and a vein which does not pass through the capillary network. AV fistula can be congenital or acquired, may be single, multiple or associated with other vascular malformations. All types of AV fistula can cause local, regional and systemic effects depending on the size, location and duration of the fistula [1]. The complications also vary depending on the degree and duration of the fistula.
William Hunter first described the existence of arteriovenous fistula in 1757 [2]. Historically, the largest series were published by surgeons who were managing war inflicted wounds during World War II, the Korean and Vietnam wars. Traumatic fistulas and pseudoanerysm accounted for 7% of the Vietnam War casualties [2]. However, most of them were treated conservatively.
Peripheral angiography is the gold standard for making diagnosis of traumatic AV fistulae [2]. Catheter based angiography can accurately demonstrate the filling of the arteries and exact point of arteriovenous communication (Figures 1 and 2) [2].
Once an AV fistula is diagnosed, an arteriovenous fistula complicating an anastomotic false aneurysm must be treated to prevent its growth, rupture, and cardiac decompensation [3].
Endovascular techniques are the treatment modality of choice because they reduce the risk of bleeding, the need for blood transfusion, the operative time, and risk of infection [4-6].
Conclusion
The endovascular management of AV fistulae is promising; it reduces the risk associated with surgery, the long hospital stay following open surgery and complications such as bleeding and infection.
References
- Saptarshi Biswas, Boris Hristov (2017) Endovascular management of penetrating zone III retroperitoneal gunshot wound injury; A case report. Bull Emerg Trauma 5: 303-306.
- Mulatti GC, Queiroz AB, da Silva ES (2013) Traumatic Arteriovenous fistula. Arteriovenous fistula diagnosis and management.
- Wolosker N, Oba CM, Espirito Santo FR, Puech-Leao P (2010) Endovascular treatment for chronic arteriovenous fistula between renal artery and inferior vena cava: image in vascular surgery. Vasc Endovascular Surg 44: 489-490.
- Junior S, Batista RRA, Felici FM, Correia VE, Oliveira MB, et al. (2014) Endovascular correction of traumatic internal iliac arteriovenous fistula with covered stent. J Vascular Brasileiro 13: 48-52.
- Tam J, Kossman T, Lyon S (2006) Acute traumatic renal artery to inferior vena cava fistula treated with covered stent. Cardiovasc Intervent Radiol 29: 1129-1131.
- Sprouse LR, Hamilton IN Jr (2002) The endovascular treatment of a renal arteriovenous fistula: Placement of a covered stent. J Vasc Surg 36: 1066-1068.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences